9 Tips for Moving from One PDSA Cycle to the Next
Congratulations—You’ve finished your first PDSA cycle, which means you have taken an essential step towards driving change. Give yourself a pat on the back and get ready to dive into the next phase of continuous improvement: your second, third and fourth PDSA cycle, or, as many cycles as needed to reach the final adoption stage.
Think about the first time you baked a cake. Did it turn out perfectly? Or did you need to try several attempts, learning and improving each time? A stand-alone PDSA cycle can rarely, if ever, result in an adoptable change idea. Instead, we rely on sequential tests that build on changes that show promise, widen the scale of testing and are performed under multiple settings and conditions.
Moving to that next cycle can be daunting, regardless of whether your first cycle went as planned. Before moving forward, remember to double check your predictions against these nine rules:
Make realistic predictions: Use the data from your first PDSA cycle to adjust your predictions for your second. Making more informed, data-driven predictions will help you better measure and understand the success or failure rates of your next cycle.
Stay on goal: Modifying an individual test of change—the original PDSA cycle—does not mean your overall project goals should change. Remember to review your answers to the three fundamental questions and make sure your change modification still supports those goals.
Update your learning questions: A new PDSA cycle means creating a new question that your test answers. Specifically, design a new question that addresses the problem noted in the previous PDSA cycle.
Identify who needs to be notified: A change to the initial test will likely impact multiple groups of people. Meeting with all key stakeholders helps ensure that the adaption will go smoothly during the Do phase of your next PDSA cycle.
Differentiate between the method and the administrator: Let’s say you have identified one element of your initial change test that needs to be adapted. For example, a new protocol did not capture as much data as expected. When considering how to adapt the protocol for your next PDSA cycle, be careful not to confuse the person (or people) who collected the data with the method of collection. Adapting the method, rather than blaming those who implement it, will lead to better outcomes.
Don’t abandon too soon: Before abandoning a change idea, reflect on your execution. Did you follow through on all steps outlined in the Plan stage? Don’t make the mistake of discarding a promising idea because of poor execution.
But, don’t adopt too soon either: When we see improvement that is greater than predicted, we can be tempted to adopt it as standard. Remember if there is still room for improvement, keep adapting and start another PDSA cycle. Stuck on next steps? Consider testing under an unlikely circumstance or increase the test’s reach.
Don’t repeat the cycle: While this may seem like a given, it can be tempting to re-test the same change if you think the results from the first cycle were a fluke. Maybe staff who had never called in sick caught a bug; maybe there was a power outage and multiple back-up generators failed. Even if an anomaly occurs, adapt the model based on the cycle’s results. In the next cycle come up with a plan for these exceptions so that you are prepared to deal with them when they occur again in the future.
Develop a robust implementation plan: Your work does not stop once you’ve identified a change idea to adopt. Provide clear instructions that include a plan for training, methods for securing resources and needed equipment, directions for revisions to policies and procedures and updated job descriptions
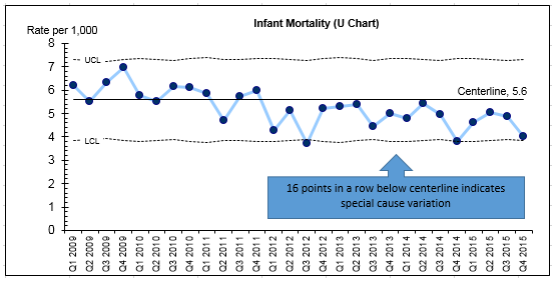
Interested in seeing these methods in action? Our free 30-minute online course, Quality Improvement 102, applies these rules to a series of PDSA cycles seeking to reduce infant mortality through smoking cessation. Take the course and continue you learning.
