Ignoring Safe Sleep Progress Risks Increasing Safe Sleep Deaths

The American Academy of Pediatrics (AAP) recently released a journal article and commentary focused on national and state trends in sudden unexpected infant deaths (SUIDs). The study concluded that national SUID rates have stagnated and this is an opportunity for states to re-examine their efforts to improve safe-sleep practices. At the National Institute for Children’s Health Quality (NICHQ), we couldn’t agree more that these statistics invite increased focus on sleep-related deaths. However, along with understanding where progress has stalled, there is much to learn from progress that has been made and take steps to leverage those successes. That is happening in many NICHQ-led, Health Resources and Services Administration-funded projects.
In the national phase of the Collaborative Improvement and Innovation Network to Reduce Infant Mortality (Infant Mortality CoIIN), a multiyear national movement that sought to reduce infant mortality and improve birth outcomes, five of 22 states that focused on safe sleep and had available data decreased their SUID mortality rates. These successes, and the work they inspired, suggest that safe sleep progress is not only possible, but has the potential to improve over the coming years and be spread and scaled to other states. Capitalizing on that potential means recognizing what has worked, ensuring that we not abandon processes before their results can be realized, and supporting the initiatives that are currently seeking improvement.
“It’s often difficult for states to access data on safe sleep death in a timely manner. Sometimes the numbers are too small and there are issues of privacy to consider,” says NICHQ Executive Project Director Pat Heinrich, RN, MSN, CLE. “We also need to remember that it can take multiple years for policy changes and process improvements, such as introducing a new educational technique, to change birth outcomes. If we only focus on the outcome measure, we risk abandoning process and policy changes that are likely to have a significant impact. Instead, we need to measure the success of process changes: Are more babies sleeping in safe cribs? Have state regulations improved? Positive process changes will ultimately result in positive outcomes.”
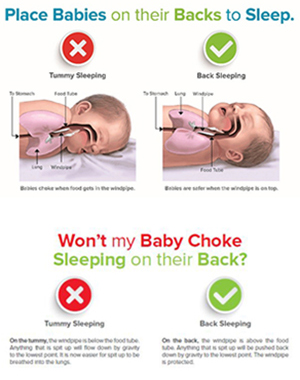
The potential impact of one such process change can be seen in New York, where the introduction of a new patient education tool has been implemented to improve safe sleep practices. Despite receiving safe sleep instruction prior to discharge from the birth hospitalization, and during post discharge home visits, New York mothers anecdotally reported being afraid of their babies choking while sleeping on their backs. In response, the New York State Department of Health adapted the NICHD-NIH anatomical diagram (see image left or click here for the full PDF). The diagram, available in English and nine additional languages, can be used as a patient education tool by providers. It is intended to help families better understand why sleeping on the back is the safest option, resulting in increased awareness of the benefits of safe sleep. The eventual impact of this will likely be substantial. The more infants who sleep in accordance with AAP recommended guidelines, the less risk of infants dying from preventable sleep-related causes.
Similar process accomplishments were introduced in other states throughout the safe sleep learning network:
- Mississippi’s Child Care Licensure updated regulations to reflect best practices to promote safe sleep.
- By leveraging methods such as crib card reminders and modelling safe sleep for parents, Massachusetts significantly increased the number of infants in the NICU in a safe crib environment.
- Another state published an interagency Memorandum of Understanding to provide bassinets and sleeping gowns to Medicaid mothers with newborn infants.
The Infant Mortality CoIIN’s full safe sleep change package—the evidence-based collection of changes shown to improve safe sleep practices—can be explored in the Infant Mortality CoIIN Prevention Toolkit. This free interactive resource provides case studies, directions and recommendations that can guide states and organizations as they seek to improve SUID rates.
“These successes provide the foundation for future improvement efforts,” says Heinrich. “The safe sleep work of the Infant Mortality CoIIN is not something that just ends with the project. This work uncovered policies and process changes that other states can now confidently adopt to reduce future sleep-related infant deaths. Our new Safe Sleep CoIIN, which gives states the opportunity to continue to refine their efforts, reflects the continued confidence the Health Resources and Services Administration has in these processes.”
The Infant Mortality CoIIN’s full safe sleep change package—the evidence-based collection of changes shown to improve safe sleep practices—can be explored in the Infant Mortality CoIIN Prevention Toolkit. This free interactive resource provides case studies, directions and recommendations that can guide states and organizations as they seek to improve SUID rates.
The Safe Sleep Collaborative Improvement and Innovation Network (Safe Sleep CoIIN), within the latest iteration of the Infant Mortality CoIIN, began in September of 2017, and is one of two NICHQ initiatives continuing to develop strategies that support safe sleep improvements. Both are funded by the Health Resources and Services Administration and both reflect the potential to use safe sleep interventions to greatly improve SUID rates in coming years. These initiatives join multiple government efforts that laid the groundwork for improving infant mortality rates and continue to have a positive effect on birth outcomes.
By 2020, the Safe Sleep CoIIN aims to decrease SUID rates by 10 percent across four participating states while significantly reducing racial disparities among sleep-related deaths. By adopting a change package that builds off the one originally developed for the national phase of the Infant Mortality CoIIN, participants identified a range of evidence-based process measures to implement, including increasing the number of safe sleep certified birthing hospitals, increasing and promoting safe sleep education, and supporting community-based home-visiting programs that leverage a safe sleep toolkit.
The Safe Sleep CoIIN and an increased national focus on improving breastfeeding outcomes has elevated the importance of connecting safe sleep with safe breastfeeding practices. This critical strategy mirrors efforts by the second NICHQ safe sleep initiative: the National Action Partnership to Promote Safe Sleep Improvement and Innovation Network (NAPPSS-IIN). This five-year initiative is expanding a national coalition working to make safe infant sleep and breastfeeding a national norm. The attention both initiatives are affording breastfeeding reflects AAP recommendations to promote better breastfeeding habits as a means to reduce sleep-related deaths.
“We are excited to bring these two health topics together and leverage the collective learning from NICHQ’s and other previous works to have an even greater impact,” says NICHQ Senior Director Jennifer Ustianov, MS, BSN, RN, IBCLC. “Together, these two efforts indicate a national commitment, a mobilization of all stakeholders in operationalizing strategies that reduce SUID rates. By prioritizing and promoting conversations that influence and support caregivers’ behaviors, we are better aligned to provide safer infant sleep environments.”
In addition to considering the barriers to progress, these initiatives invite a conversation on the progress that has been made, what this progress indicates, and the steps now being taken to leverage that progress and help more babies celebrate their first birthday.
Let us know if you want to get involved. Sign up for our mailing list to stay up-to-date on the project’s work.
