Insights
Why Closing the Health Equity Divide Can’t Wait Any Longer

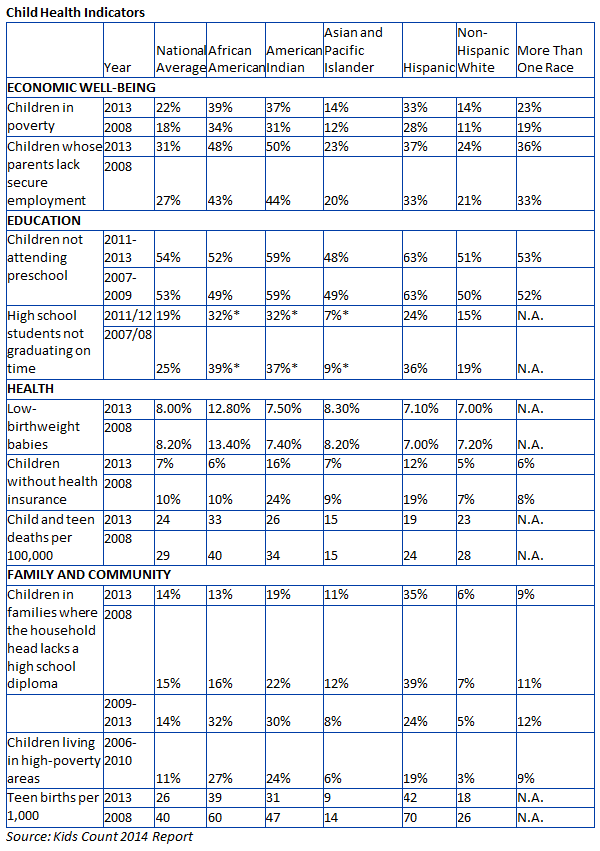
It’s encouraging to see that four main child health indicators—economic well-being, education, health, family and community—continue to show overall improvements (see chart pg 17). However, the key indicators continue to also show disparities based on race and ethnicity (see chart below). With the projection that more than half of the nation’s children will be part of a minority race or ethnic group by 2020, the need to address health equity has never been stronger.
Equity in healthcare is the idea that everyone has the same access to quality care, regardless of social, economic, demographic or geographical differences. This ideal is not a current reality in the U.S. healthcare system. There are many barriers hampering health equity and the overall health of America’s children. Here are just a few:
- Access to Care: The fate of the Children’s Health Insurance Program (CHIP) is unknown after 2017. CHIP provides coverage for uninsured children in low income households but above the cut-off for Medicaid eligibility. Decisions about CHIP’s future will be consequential as more than 8 million low-income children were covered by CHIP at some point during 2012. CHIP and Medicaid combined cover more than one in every three children in the U.S. The percentage of Medicaid/CHIP-covered children identifying as something other than white, non-Hispanic, grew just 2.7 percent from 2000 to 2010. However, the share of Hispanic children increased by 6.7 percentage points overall, from 16.3 percent in 2000 to 23.0 percent in 2010; also white children steadily remain the largest racial/ethnic group receiving benefits, while their share of the total population declined by 7.7 percentage points.
- Income Distribution and Poverty: Income distribution in the U.S. has changed drastically. Income inequality in the U.S. is greater today than it was prior to the start of the Great Depression in 1929. A third of children in the U.S. live in poverty, a known risk factor that influences childhood development and health outcomes. African Americans, American Indians and Hispanics have the greatest percentage of children living in poverty.
- Fertility Trends: The age of women at their first pregnancy is rising, along with the pregnancy rate for women 30 and older. Pregnancies at advanced maternal age (over 35) have more potential complications. Non-Hispanic black women, whom have the highest pregnancy rates overall, are seeing age at first pregnancy increase too, which is concerning given this population already has the greatest disparities when it comes to infant mortality rates.
How do we work to achieve health equity? How do we reduce the health disparities we see among race and ethnicity? The answer is complex. It’s not as simple as making sure every child can easily access and receive high-quality care regardless of zip code or family bank account balance. It’s not just about access. Addressing children’s health equity will require a culture shift that addresses the competing priorities that make it difficult to achieve true progress in the U.S. healthcare system. It will require taking a close look at the root causes, in particular, social determinants of health such as poverty, education and others, and putting in place both short-term and long-term system changes.
Change isn’t easy. Working at NICHQ—an organization where systems improvement is our business—I’ve seen firsthand how hospital teams, primary care physician offices, community-based organizations and even state health departments can struggle while making meaningful and sustainable improvement to their programs and services. It’s not for a lack of desire, ideas or means; mobilizing innovations when there are so many competing priorities for our time and attention is arduous.
Now—right this minute—is the time to put health equity first. In just a few years, children of a minority race or ethnic group will make up the majority in the U.S., which means, if we do nothing now to stop the current trends, the overwhelming majority of U.S. children will experience sub-optimal health outcomes. That’s not the country I want to live in. What about you?
Cindy Hutter, MBA is the Director of Marketing and Digital Strategy at NICHQ
